Free Webinar · May 7 · How to Get (and Keep) More Patients as a Practitioner →
Save Your Spot
Table of Contents

Experience Better Practice Management Today!
Starting at $28.05/month
No Credit Card Required

Experience Better Practice Management Today!
Starting at $30/month
No Credit Card Required
From what I have seen across clinics, the first three osteopathy sessions often shape whether a patient continues care or quietly drops off. Long before major results show up, patients are already deciding whether the plan makes sense, whether the practitioner understands their problem, and whether each visit feels connected to the last one.
In this blog, I’ll break down what osteopaths should focus on in those early visits to improve follow-through and keep patients engaged in care. That usually comes down to a few things done well:
Let’s start with session one.
Retention improves when the practitioner identifies what the patient wants back in daily life, not just the symptom being described.
A patient may come in with neck pain, headaches, stiffness, fatigue, postural strain, stress-related tension, or recurring discomfort. But what usually matters more is working comfortably, sleeping better, moving without fear, or getting through daily life with less effort.
The first session should uncover:
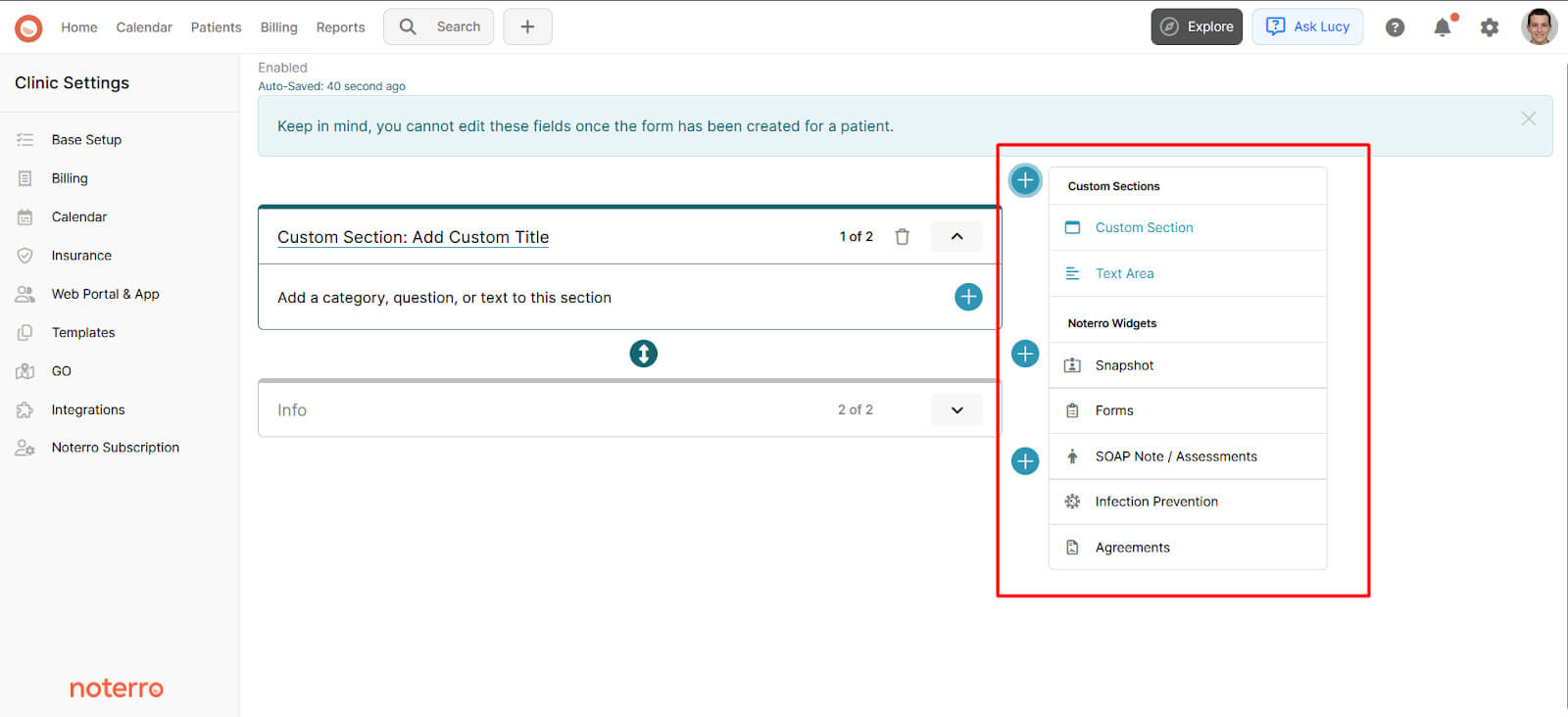
That only works well when those details are captured properly from the start. Noterro helps here by letting osteopaths customize intake forms before the visit and create custom note templates that go beyond standard S, O, A, and P fields. That gives them better context early and makes it easier to carry that context into future sessions.
You might also like: 10 Best AI SOAP Notes Tools for Osteopathy Clinics in 2026
After that, the practitioner needs to explain the case in language the patient can follow easily. That explanation should use simple language, not jargon that sounds impressive but adds confusion.
When the explanation is easy to follow, the patient is more likely to understand the reasoning behind the plan and take the next step with more confidence.
The first session should also set a realistic picture of what progress may look like. Some patients expect major relief after one visit, while others assume early improvement means they no longer need follow-up.
That is why expectations need to be set early and explained clearly. I would outline:
I would also explain what the patient should notice before the next visit, especially when progress shows up in smaller shifts before it becomes more stable. Patients do not need guarantees, though they do need clear direction.
The first session should close with a specific reason to return, not just a general recommendation to "come back next week."
When a new patient leaves without understanding why the second visit matters, they will weigh it against everything else competing for their time. Other priorities win more often than you would expect.
Before the patient leaves, tell them exactly what you found, what you are treating, and what you expect to change between now and the next session. If you are planning a reassessment at visit three or four, say that too. Patients who understand the arc of their care are more likely to follow it.
A useful close sounds something like this: "Based on what I found today, I want to start with your lower thoracic mobility and the left hip restriction. By your second visit, I would expect some reduction in your morning stiffness. At visit four, we will reassess your range of motion and decide whether we need to adjust the plan."
That framing does three things. It gives the next visit a clinical purpose. It sets a measurable expectation that the patient can actually notice. And it positions the reassessment as part of a plan rather than an open-ended commitment.
When the purpose of the follow-up is vague, patients do not necessarily decide not to come back; they just do not book right away. And that gap is usually where attendance falls apart.
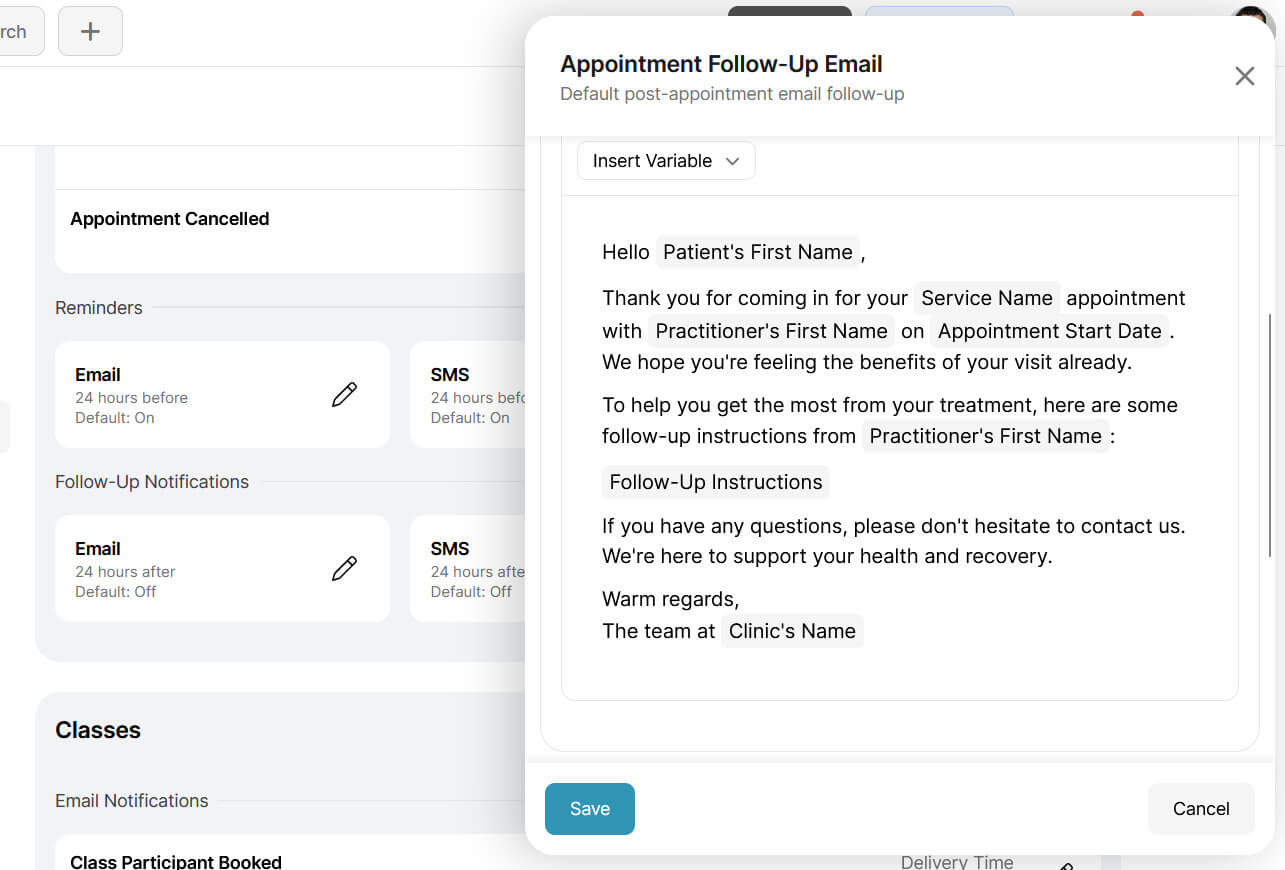
Closing the session with a defined next step and making it easy to book before they leave removes that gap. Noterro lets patients book their next visit during checkout through a clinic-branded web app, and automated follow-up notifications can reinforce the purpose of the second session so the clinical context does not fade between visits.
Also read: What to Look For in Osteopathy Software That Improves Patient Experience
The second session should pick up where the first one left off. If the patient has to repeat everything again, the care process can start feeling disjointed.
The second session should review:
Small changes still matter when they are explained properly. Better sleep, less morning stiffness, or greater confidence in movement can indicate progress even when symptoms have not changed dramatically.
Those details should be easy to review before the session. Noterro helps by showing a patient snapshot upfront, while chart notes, intake details, and treatment history stay together under the patient profile.
Repeating the same treatment without explanation can make care feel routine. Even when the approach is still appropriate, you want the patient to understand why you are continuing it or changing it.
The discussion should explain what is responding well, what still feels limited or sensitive, and how the patient’s feedback is shaping the next step.
That shows the patient that the plan is being shaped by their response, not repeated by habit. It also makes the clinical reasoning easier to follow.
Pain scores can help, though they should not carry the whole progress review. I would encourage you to look at what the patient can do more easily in daily life, because that usually feels more real than a number on a scale.
You should check if your patient can sit longer, bend more easily, wake up with less stiffness, or get through work with less fatigue. You can also ask whether:
That usually gives you more useful outcome measures and helps the patient see progress in a way that feels practical. Function-based progress often builds more commitment than symptom language alone.
By the second session, some patients start thinking they can stop early because symptoms are easing. This is where I would explain what has improved, what still needs work, and why stopping too soon can interrupt progress.
I would keep that explanation tied to something the patient already notices, such as lingering restriction, lower tolerance under load, or improvement that still feels inconsistent. That gives the next visit a clear clinical purpose instead of making it sound like a routine rebooking.
Bonus read: 10 Best Osteopathy Practice Management Software for 2026
In future sessions, patients usually need help seeing both progress and what still needs attention. Once symptoms start easing, many forget how limited they felt at the beginning, so I would compare their starting point with how they feel and function now in a simple, structured way.
That comparison should show what has improved, while also explaining what still feels unstable, restricted, or not fully resolved. I would also explain the difference between early relief and lasting stability in a calm, evidence-based way, so the patient understands why continued care may still be useful without making the conversation feel dramatic.
The conversation should shift from an early response to what ongoing care should look like for this specific patient. A general recommendation is usually not enough at this stage because the patient now has enough experience to judge whether the plan feels relevant to real life.
I would shape that next step around:
This is also the right time to tighten home care advice so it feels realistic to follow between visits. Patients are more likely to continue when the recommendation feels built around how they actually live, not just around the condition itself.
Helpful read: Why Soft Skills Are Essential for Client Retention in Allied Health
Retention in osteopathy begins to take shape in the first three sessions. When those visits feel clear, connected, personalized, and clinically grounded, patients are much more likely to stay engaged.
If the patient understands the problem, can see progress in daily life, and knows what comes next, continuing care feels more reasonable and easier to commit to. That experience also becomes easier to deliver consistently when tools like Noterro help keep notes, context, and follow-up steps organized from one visit to the next.
Tie the recommendation to something the patient already noticed, such as lingering restriction, uneven progress, or difficulty under normal daily load. When the reason is clinical and specific, it sounds useful rather than pushy.
Keep the plan realistic, offer practical spacing, explain which timing matters most, and make booking easy before they leave. Short, clear follow-up messages also help when their schedule changes often.
They can explain the problem in simple terms, know what progress to look for, understand why the next visit matters, and follow home advice with reasonable consistency.
Set a clear structure for the first couple of visits, standardize what should be covered in each one, and review notes or recordings to coach for consistency in explanations, goal-setting, and follow-up.
Do not stop at that first answer. Ask about sleep, stiffness, movement, work tolerance, and confidence with daily tasks. Small changes often show up there before the patient sees them as progress.
Reach out quickly with a simple, supportive message. Remind them what the missed visit was meant to review, make rebooking easy, and keep the tone helpful rather than guilt-driven. With Noterro, clinics can send cancellation email notifications automatically and use that moment to prompt patients to book a replacement appointment instead of letting the gap continue.
Tags



